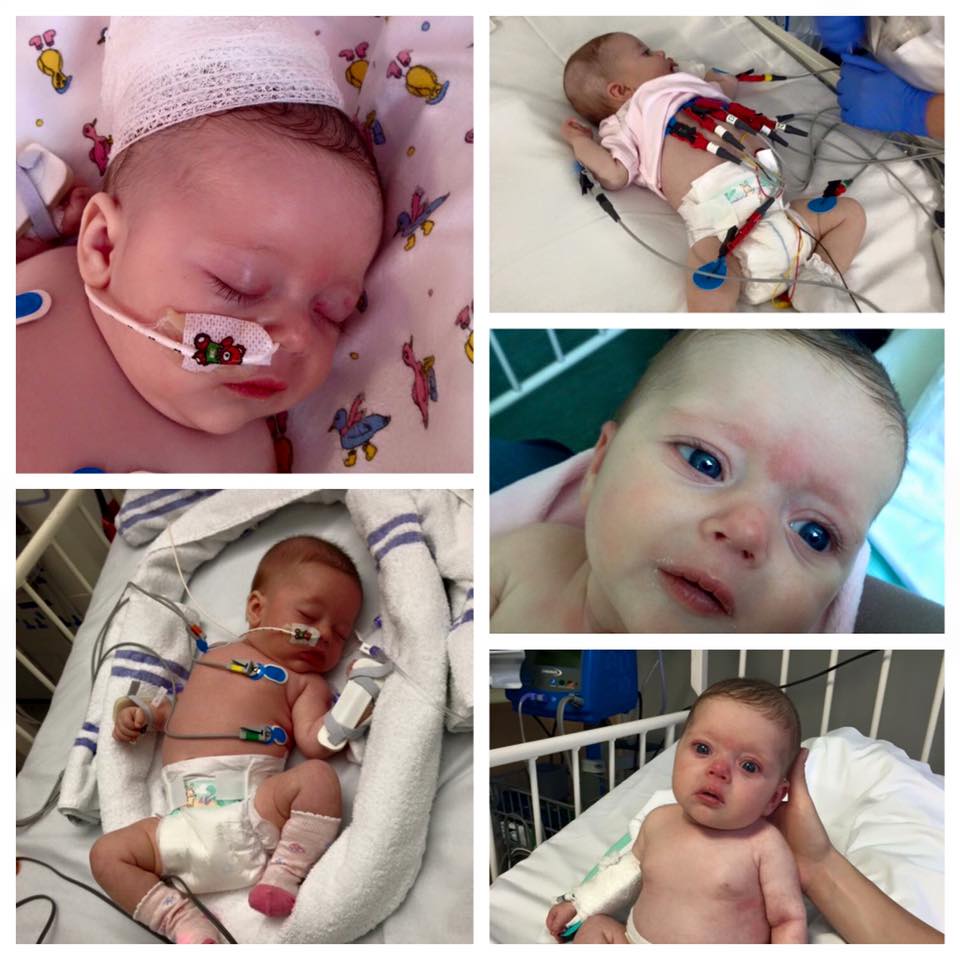
Dear Freya,
So, we finally acknowledged that angiogram shaped elephant in the room, and on Wednesday 21st February 2018, almost 2 years to the very day that the ‘A’ word was first mentioned to us, you underwent cardiac catheterisation at Leeds General Infirmary. And you are still here! Woohoo! I could feel all the fear and worry that has burdened my shoulders for the last few years lift off and evaporate in the waiting room the moment I saw the Cardiologist’s face as he walked towards us, smiling.
Let me tell you about the day so you can read about it when you are old enough to understand what you have been through. Although I feel that somehow instinctively you know, because you have not stopped squealing “Woohoo!” since we got home!
Our day started at 6am, when I woke to my alarm with a sinking feeling in the pit of my stomach. ‘A’ day had arrived; a day I had been dreading for so long. Before I woke you, I called the hospital ward to check they were expecting you and that they still had an available bed. “Yes, we are expecting Freya,” said the nurse, and my heart sank. I climbed back into bed with Daddy, and cried quietly as I let it sink in. I know it had to happen, but I was as disappointed that it was going ahead as I had been at it being cancelled a few weeks before. It was indeed a necessary evil; we wanted you to have it, but we didn’t want you to have it. But now we just needed to get on with it, and have hope. I put the angel wing earrings in that our friend had bought me, and although I don’t think I am a religious person, and I am not a Catholic, I will admit I popped the rosary beads that I had bought in The Vatican into my bag!
I woke you up, and after you’d sleepily been to the toilet, I wrapped you up in your dressing gown and put you in the car. Our overnight things had been packed the night before, as we were told to expect to stay at the hospital. You weren’t allowed anything to eat or drink after midnight the night before, so we were surprised when your first words weren’t, “I need some brukfust!” like they usually are! I guess the whole routine was different to you. As usual, and despite being rudely awakened at 6am, you were happily chattering away in the back of the car, telling us about everything you could see on the journey up, and repeatedly saying, “We love you, don’t we Mummy,” which just made my heart ache. It struck me as strange that you used the word ‘we’ and I got this odd feeling that somehow we weren’t alone, us three, on that journey.
When we arrived in Leeds, Daddy dropped us off at the doors and went to park the car so that we wouldn’t be late. Although we visit this hospital regularly for your follow up appointments, I felt my stomach lurch as we walked in. Usually your appointments are in the Outpatient’s Department, but this time we would be going back to Ward L51 in the Clarendon Wing – the ward where you were admitted when the Children’s Hospital had you transferred up there for specialist cardiac care. We entered the ward, and right ahead of us was the high dependency unit that you had shared with post-op babies with vertical scars down their chests. I had been so focussed on the procedure itself that I hadn’t considered how it would feel to be back there.
We were ushered into the playroom, where within minutes the Doctor had arrived. He was in blue scrubs and he spoke in a calm and kind way that put me immediately at ease. He explained that you would be his first patient of the day, so you would be going down for your procedure at around 9am (it was 7:30am when we arrived). He gave me a brief outline of what would happen, and explained the risks in such a way that I didn’t feel afraid of them anymore. He said that both me and your Daddy would be able to go into the room when you were given the general anaesthetic, which made me really happy as the last time you were put to sleep I had to go through it on my own. With every sentence the Doctor spoke, I began to feel stronger. Daddy then arrived, and the Doctor took the time to repeat the information to him, and I signed the consent forms. He said that if everything went as they expected it to, we should be able to go home that afternoon. He also said that the day needed to be as fun as possible, and that both the hospital staff and us were to concentrate on that, for your sake. He said, “This doesn’t have to be frightening for Freya, she just needs to think that this is normal.” I didn’t think it was possible for us to do that, but as you will read, we all pulled it off!
Shortly after the Doctor left, a nurse arrived to show us to your bed. As we were headed towards your bay, the nurse said we just needed to nip into a side room to check your weight and height. I looked around the room, trying to figure out why it felt familiar. It looked smaller than I remember it. More cramped. And yet the last time you and I were in there, it was full of medical professionals and the ambulance crew were poised in the corridor, waiting to see if you would be taken back to Sheffield. They were sent away. I can remember Dr Brown (your Cardiologist) sitting by the side of the bed preparing to do an echocardiogram. I don’t remember any of the other faces, just that they looked intrigued, serious and concerned. And I remember I was in such a heightened state of panic as you had got so hot in your car seat strapped to the ambulance gurney and your fever still hadn’t abated after 17 days. For a moment, it was like I was watching it all again, like a kind of out-of-body experience, but then you needed help to get your back straight against the wall so the nurse could record your height, and I snapped back into the moment.
Within minutes of arriving at your bed, two members of staff came to see you. One was the Anaesthetist and I can’t remember who the other lady was. I was surprised at how they addressed you to explain to you what was going to happen. I remember thinking, “She’s only 2! She can’t understand what you’re saying!” but I realise that they were building trust and forming a relationship so that the experience would be easier for you. They said they would see you soon for a little sleep, and just in case you didn’t respond well to the breathing mask they put some numbing cream on the back of both hands with a clear plaster to cover them. Although you giggled at the coldness of the cream, you didn’t like it much and we had to tell you we had the cream on too to convince you to get the other hand done. They wrapped your hands up in bandages so you looked like a boxer, and the probe on your finger lit up so you looked like ET (you won’t know who that is, but we will watch the movie one day).
When they were done, the Play Nurse arrived! Her name was Gemma and she was wearing a bright yellow T-shirt. She had a big bear with her, I can’t remember his name. He had a cannula in one hand, and a clear plaster on the other, and the nurse was carrying a green mask. She gave you the bear to play with, talked to you about the cannula and let you play with it, and she gave you the breathing mask to play with too. Me and Daddy played with the mask as well – we put it over our mouths and pretended to fall asleep, snoring! You thought that was funny, and you helped put the teddy to sleep too. After you’d had a chance to play with the teddy, and Gemma had talked to you about your procedure, she asked what you would like to do next. You chose to do some painting, so all three of us sat at the little table and painted together. As the time passed by, it didn’t feel like we were waiting for anything at all. It just felt like you, me and Daddy spending some lovely time together! Personally, I found the painting quite relaxing, and I couldn’t believe it was 9am already when another nurse came through to collect you. They were ready for you.
You didn’t want to stop the painting, but we explained that there was somewhere exciting we needed to go, and that you were going to have a little sleep. You could come back to do some more painting later. So off you skipped down the corridors, stopping every now and again to look back and ask us which direction we should go in. We went down in the lift, and walked for ages until we finally reached the Cardiac Catheter Lab, which was through some red double doors. We went into a room on the left, and could see the Doctor and another member of staff behind some glass. It looked like the kind of operating theatre that you see on TV hospital dramas, and Daddy and I were surprised by how many people were in the room. I was expecting to lay you down on the bed like the last time, but instead they asked me to sit down in a chair, with you on my knee facing away from the bed. I guess when you last went under general anaesthetic you were just a tiny baby, and you were so sick that you really didn’t put up a fight at all. This time, with you being so much more aware, I guess this was the better way. When they held the mask over your face, you didn’t protest. How clever that they introduced you to it earlier on, so now you just accepted it as normal! They asked you to breathe, and to try and blow up the balloon that was attached to part of the tube. You started to feel heavier in my arms, and at one point you started to throw yourself about a little. The anaesthetist said not to worry, that it was the general anaesthetic working and was quite normal. And then you were asleep, which I knew because you started snoring really loudly! I’ve never heard you snore like that before, Pickle! I laid you on the bed, and they said we could give you a kiss goodbye before we had to leave. Daddy leaned in and gave you a kiss, and then I did too. I’ll admit that is when I began to cry. We had been so strong for you, it wouldn’t do any harm to let it out now that you couldn’t see us. They told us to come back in 30-40 minutes, and we had a feeling it could be one of the longest 40 minutes of our lives.
Daddy and I went down to the hospital entrance to get a coffee and some breakfast. Daddy said he felt bad getting a bacon sandwich when you hadn’t eaten, but I told him it was okay because you didn’t know! Standing in the Costa queue, I turned to your Dad to ask if he was okay, and he was really upset. We don’t often see your Daddy cry, but seeing your child get put to sleep is not a nice thing to go through, and it really hit him. We sat and ate, and I just felt an overwhelming sense of sadness over our situation. This had never been in any of our plans, and here we were drinking coffee, in a hospital surrounded by Surgeons and Doctors and Nurses on their breaks, while somewhere upstairs your life was in someone else’s hands. I felt helpless, and heartbroken that you were having to go through this at all.
After what felt like 58 million hours, we decided to come back to see if your procedure was over. My heart jumped up into my throat every time those red double doors opened, but it wasn’t long before your Doctor came through them and walked towards us with a smile and a nod that seemed to stop time. He sat down beside me and your Daddy and said that the procedure had gone really well, and then he said it. Your arteries look “pristine”. That is the exact word he used: pristine. Now if you don’t know what that means, and for the purpose of illustrating just how amazing this news is, let me share this with you here:

Unspoilt, perfect, immaculate. Just like you.
We couldn’t believe what we were hearing. Daddy said “It’s what we wanted, it’s what we wanted!” as the Doctor told us that everything looked normal, and they could see no signs of any damage at all. Normal! Do you hear that! He said he would keep you on the daily aspirin, but I said that your Cardiologist was keen to stop it if there was no need to continue. He agreed that there was no real evidence either way, so the decision would be as much led by us as by the hospital, and we decided we would wait to see what Dr Brown would like to do. I said I had not expected to hear such amazing news, and wondered if the fact that you were so young at diagnosis had anything to do with the outcome. He agreed that babies, and young children, are remarkable healers. He said that you would need to go back in the future for a stress echo, but for now everything was just fine! You were waking up, and a nurse would come out to collect us when they were ready.
When the nurse came out and lead us through the red doors again, we could hear you screaming. We entered the recovery room, and there you were, confused and upset and fighting with the staff who were trying to apply pressure to the entry wound to stem the bleeding. The more you struggled, the harder you made it for them, and you were writhing about on the gurney trying to get away. It must have been frightening for you, and I am guessing it might have been hurting too. I’ll admit I wasn’t prepared for the recovery. I hadn’t expected to find you like that, and both me and Daddy went right into action to try to help you. You were calling for us, and we were reassuring you that we were there, but you were in such a state. You asked for a cuddle, so Daddy held you on his knee in a chair whilst the nurse tried to keep the pressure on your groin area, where the catheter tube had been inserted. Then you started calling for me, and Daddy passed you to me, but you were still very unsettled. And then the nurse said they had to get you laid down again as you were bleeding out, and I looked down and saw the blood stain spreading across my cream jumper (my favourite jumper might I add!) Then I panicked, and I cried, and I said “It’s my fault, it’s my fault, I wasn’t holding her right!”, and they told me not to worry, that they expected the bleeding, and it wasn’t the first time it had happened. In fact they apologised to me for the state of my clothes, but I really didn’t care, sweetheart, a jumper can be replaced. The Doctor who performed the procedure came back in to help, and eventually the bleeding must have stopped because they called for a porter to come and take you back to the ward. It was hard to see you so upset, and us not be able to offer much comfort. Most of the journey back to the ward, you were calm, but then we would stop to open a door, or call a lift, and you would start crying again. I wonder what was going through your mind. I reminded you of the CBBC Get Well Soon video we watched where Dr Ranj was singing about a bed with wheels, and you smiled a little at that.
We were soon up on the ward again. They told us you wouldn’t be able to eat for a while, particularly as vomiting can be a side effect of the anaesthetic, but that you may want to have some sips of water because your throat may be sore. We had to get you to lie flat for a number of hours – how do you manage that with a toddler! But actually you were pretty whacked out by the experience, and you did lay there with your favourite teddy, the teddy that had stayed with you in the theatre when they did the angiogram. I budged you over on the bed, and snuggled up beside you so we could read books, which I held above our heads until my arms ached! You kept sending Daddy back and forth to the library to fetch new books, and he kept going because it was the least we could do to keep you happy after what you had been through. My advice to a parent going through this with their child to pick lightweight books! You wouldn’t have wanted to hold the book yourself – you were too busy sucking your thumb on one hand, and fiddling with Pink Teddy’s ears with the other! You had a probe attached to your foot to monitor your heart rate and oxygen levels. I watched the numbers on the machine, and noticed the stark contrast between the monitor then, and the constantly alarming monitors of 2015. My, how far you have come!
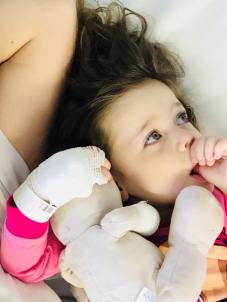
I guess it was around 11am by the time we had got back to the ward, and you still hadn’t eaten anything since 6pm the night before. You were getting hungry, but it was too early to eat so we told you that your lunch was cooking, and distracted you with more books. Whenever a nurse walked by you would shout out, “Doctor! I’m starving!” Soon enough it was lunchtime, and being a paediatric cardiac ward the offering was jacket potato and baked beans, the suggestion of which was met with a rather indignant response from you, and a request of “Have you got any cheese sandwiches?” Despite not usually serving that, the staff went off and came back with a plate of cheese sandwiches, a yoghurt and a banana that they had made to look like a dolphin. They all made such a fuss of you, and all the staff said you were very cute. You even made a friend – 8 year old Emily who was waiting for open heart surgery. Once you had eaten and you were able to sit up, it was like you hadn’t been through anything at all. You were back to being your usual self, a cheeky little chatterbox, charming everyone that you met! The rest of the afternoon was pretty uneventful, and because you could sit up you were able to open the gift that ‘La La Lis’ had sent with us, with treats and activities inside, which kept you busy for a while.
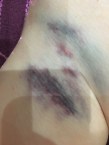
The Doctor came to see us again in the afternoon, to say that he was happy for the nurses to discharge you when they were ready. You had recovered well, and the only sign of what you had been through was the nasty bruise in your groin that w
ill probably be there for some time. He repeated that everything had gone really well, and that your heart looked perfect. He mentioned the stress echo again, and we asked how old you would need to be for that – he said at least 8 years old. I asked about CT Calcium testing as I know that research has shown that the presence of calcium in the arteries can indicate risk of further complications, e.g. heart disease. This test is recommended 10 years post-diagnosis, as calcium can take years to build up. The Doctor did mention the ‘D’ word (discharge), but I quickly jumped in to say that I would expect you to be followed up for life, and he didn’t argue.
And so, around 5pm, after a long but strangely fun day, we were told we could go home. I asked Daddy to go and get the car, and I would meet him around the front of the hospital; there was something we had to do…
On Friday 18th June 2015, as we were leaving the Cardiac unit to return to the Children’s Hospital following your week on the HDU, I made a visit to the hospital chapel. Your Auntie had mentioned that she wanted to leave a prayer before we left, but we were discharged before she got the chance. So I decided to do it for her. The day before that we had been told there was a chance we could lose you, so I knew what I wanted to write on my prayer slip. Dear God, Prove them wrong.
On the 22nd February 2016, your Cardiologist told us that they wanted to do an angiogram, and the start of a worrying two years began. That night, I wrote a blog, where I shared a photograph of the prayer slip along with these words:
“Somewhere in there…there is a tiny voice of hope…She sounds how I imagine Freya to sound in a year or so. I see those eyes through the fog too. They are looking at me, huge and wide, and they are saying “I’m going to be ok, Mummy.” This kid is miraculous. She is made of something stronger than you and I were made of. Maybe, just maybe, she is going to prove them all wrong…”
And on the 21st February 2018, after we had faced the elephant in the room, and survived, you and I went to the chapel together. I took a blank prayer slip from the table and wrote what I needed to say. And then we walked up to the altar and both of us said out loud, “Thank you.” And we meant it from the bottom of our perfect hearts.
We also left a note on the prayer tree for the research team
Our journey with Kawasaki Disease is not over, we have merely reached a pretty big break in the road. The distance between the follow up checks will become greater, perhaps 5-yearly from now, and we will have a number of years to wait before the further tests (stress ECG/echo, Calcium CT test and perfusion scanning) are undertaken to ascertain the risk of long-term effects on your heart. Although the remodelling process can be excessive and lead to narrowing (stenosis) at a later stage, we remain cautiously optimistic for your future. We know you are at greater risk of heart disease and will do our best to protect it, as the doctors have advised; healthy eating, no smoking, and get you into an activity now that will keep you physically fit into adulthood – cycling, running, swimming or dancing. Oh yes, there will be lots of dancing!
I e-mailed a number of the Kawasaki Disease specialists who have been on your KD journey with you from afar, including Professor Jane Burns (World Leading Kawasaki Disease Specialist). Whilst they all celebrated our news, the cautionary notes were still clear. “Make sure she has ongoing and long term follow up and that no one is tempted to discharge her!” was the note from one of the specialists, and another said “While I hope the later narrowing will not occur – it is important to be aware that it’s possible and arrange long term follow up.” Jane didn’t need to say any of that, as she knows me too well, and knows that I will never stop advocating for you and the disease, so this is how she received your wonderful news:

You can count on it Jane! Whether we like it or not, we are part of a wider family now, and we will never stop campaigning to raise awareness of this disease. Freya’s 3rd birthday party fundraiser is on the horizon, and we can only hope that whatever amount we raise can make a difference to the research programme. For now though, our family can focus on that ‘normal life’, although I am not sure I am satisfied with ‘normal’. No, for us I want an extraordinary life, and the hope that we have gained from seeing that sometimes you can believe in miracles might help us do just that.