I have just returned home from handing back all my equipment to my employer as I embark on this new chapter in my life. Funny how strange it felt handing back a laptop and a mobile phone that have only been locked away in the garage for the last year anyway. I guess it felt somewhat symbolic of the final step towards (temporary) detachment from my career. And just being there in the restaurant, drinking coffee like I used to every morning when I was there, felt quite surreal. More so, because I had you by my side, and a rice cake in my hand instead of a notepad. I was very aware, having just finished a year of maternity leave, that under normal circumstances I would have been there alone. I would have been the one rushing off to that conference call, or heading off to a meeting. I have no regrets, however. Non, je ne regrette rien. I consider myself incredibly lucky to have the chance to take some additional time to concentrate on your immediate needs, and to regain some of the time we lost last year. With your brother and sister I would have missed so much of what I get to see every day with you sweetheart. Watching you develop and grow is a source of constant amazement for me, and I don’t think I will ever tire of spending time with you.
The effects of the last year were not just felt by me. I’m sure they were felt by you, but I have no idea how because you can’t tell me yet. I hope that you don’t remember any of it. That all you remember is how we used to go on the train for days out, or for coffee and cake and to the park. I won’t ever forget that the backdrop for all of those things was an imposing hospital looming behind us. But hopefully you will just remember feeding the ducks in that nice park, and you won’t have noticed the tears in my eyes that came because I was saddened by the memories that the park evoked. One day we will be able to go to Weston Park and sit on a bench and let the warm sunlight wash over us as though it were sent right from Heaven. We will lie on a blanket and make pictures in the clouds, feed the birds and the ducks and watch the fish in their shady hiding place under the little bridge. But we will always make our place on the other side of that park so as to spare the mums who, like me last year, watched other families enjoying the summer through the windows of a hospital cubicle. The nurses thought they were helping me by moving me to a room with a view. The brick wall which was our previous view had been quite oppressive, but no more so than watching mums play with their babies in the shade of the trees.
Back then I thought I did a pretty good job of protecting your brother and sister. We told them that you had a cold but needed the nurses to help get you better because you were too young for Calpol. It was a white lie. Quite a big one, but white nevertheless. And you did test positive for Rhinovirus in that first week, so it seemed like a plausible excuse. We also kept your siblings from the hospital. They visited you on your last day at the local hospital (after a week), and then maybe once or twice when we moved to the Children’s Hospital. We didn’t tell them when you were moved to Leeds, so they didn’t see us when I was in my darkest place. What I didn’t know was that our attempts to protect them probably made their anxiety worse. I underestimated Eliza. She has told me since that she was very worried that I would be coming home without her baby sister. She wasn’t stupid; she knew something must be pretty wrong and that a common cold wouldn’t need her mum and sister to be away from them for as long as we were. So she actually worried more, because she knew it had to be bad for us to want to hide it from her. And Fin? Well he went off the rails a bit. His behaviour at school hit an all time low, and the effects of last year have only just begun to wear off with a huge amount of support from the school. He was the baby of the family before you came along, you see. He was excited about getting a baby sister (although I do think he might have secretly been hoping for a brother to play Minecraft with!), but suddenly not being the baby anymore is quite a lot for any child to get used to. And then just 7 weeks after we brought you home, just as he was probably getting used to you being around, he lost you and me for a while. 6 weeks. That’s a long time in a 5-year old’s life. Because we played down your illness so much, he couldn’t understand why his Mum would leave him. He thought that I had chosen you over him, and his little head wasn’t quite ready to work that one out. His self-esteem took a huge knock, and he became very insecure for a while. No need to feel any guilt about that though, not you or I. I made the decision to protect them for all the right reasons and I wasn’t ready to tell them that they might lose their little sister. They didn’t need that worry. And by the time you read this, you will have seen that none of this had a lasting effect on them; they probably won’t even remember it when you’re old enough to be reading this.
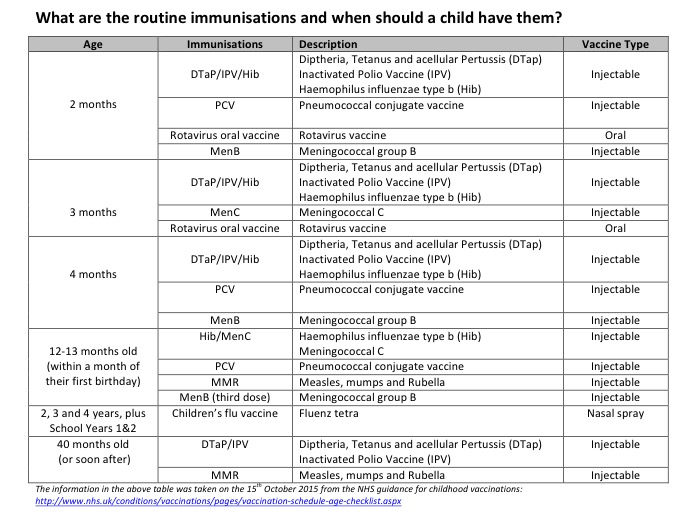
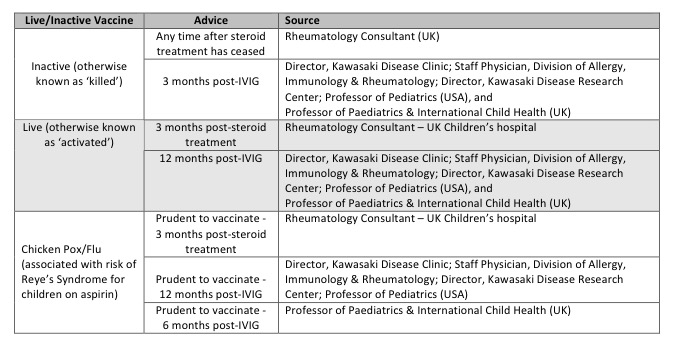
I am not the same person that I was before I had you. I might even go as far as saying that you are lucky that this happened to you. You have had the very best of me this last year, and I dare say that you will continue to get the best of me for as long as we are both here. I have not taken a single moment with you for granted, and because of that I think I am more patient with you than I might have been with the others. I am most definitely more intuitive about your needs. Perhaps some of that is due to age (I was 40 when I had you), or experience with having done it twice before. But I think most of it is the incredible bond that we have developed by spending so much time together since you came into the world. Because I am scared of you getting very poorly again (I’ll tell you one day about chicken pox and the medication that you take), I have kept you away from large groups of children in the main. I don’t take you to baby and toddler groups or play areas where the risk of infection is a constant worry for me. I don’t wrap you up in cotton wool either – rather than avoid all situations, I tend to weigh up the situation based on my anxieties and I guess you could call it damage limitation, rather than complete avoidance. That will become easier towards the end of this year (2016) when you have received the MMR, Chicken Pox and Flu vaccines. Until then, we will stay together in our little bubble where we see just the right amount of people to allow you to build relationships with other children, but not enough for me to worry about you becoming sick. I know I cannot protect you from everything, but I have to protect you from what I see as a risk, no matter how small that risk might be. I cannot bear the thought of seeing you that sick again, Peanut.
My social circle is a little smaller than it used to be too. There are lots of reasons for that. I’ve become very immersed in a Kawabubble over the last year and I don’t have an awful lot of time and energy for much else. Most of my attention is on you, and getting you through the next challenges that the effects of KD will throw at us. A lot of my attention has turned to our little family; this experience has made my family much more important to me than I think I allowed it to be before. It’s also very difficult for me to spend time with people who cannot relate to our situation. I don’t want constant sympathy, but I want compassion and understanding. People that think that everything is ok now because I wear a big smile, and you look so amazing, don’t know me very well. They don’t know how much I still struggle to come to terms with what has happened to you, and what the impact of the disease will have on your future. 70% of children in your situation will have to have invasive treatment later in life – a heart bypass, or a stent perhaps. 100% of children who have suffered coronary aneurysms as a result of KD will suffer myocarditis (inflammation of the heart muscle) which causes degeneration or death of heart muscle cells. I don’t know how to compute the possibility that my child may show symptoms of myocardial infarction (a heart attack). Just doesn’t seem real. Later this year, whether it be through cardiac catheter angiogram or CT angiogram, we should get a closer look at the cause of the remodelling of your coronaries to better understand what the future may hold. Right now I have to take the cues from your outward appearance and development, and you look mighty fine to me. It’s very confusing though. I’m still not sure if there is any chance that you could have complications today, tomorrow, next week. I guess we have to take each day as it comes.
I don’t want people to think that I am a victim in all of this. That I don’t want to let go of it. In fairness, I can’t let go. Partly because you are still affected by the disease and will be for many years to come. Partly because I feel I have gained a purpose; I can help make things better for other sufferers of the disease, whether it be through raising awareness to help speed up diagnosis, or by providing useful information to other parents going through this. Kawasaki Disease is now a very big part of my life, of our lives, and it isn’t likely to go away. Perhaps over time it will become a smaller part of life for all of us, but I don’t think I will ever stop talking about it to anyone who will listen (and a few who don’t!). It’s too important for that. I am in contact with parents and grandparents who have seen this illness first hand, some who have suffered the worst consequence of all. For them, I will always do what I can to help change the future of Kawasaki Disease.
Having a child diagnosed with a rare, or little known, disease is life-changing for parent and child. And when there is no known cause you never stop asking yourself ‘Why?’. Why did this happen to you? I hope we find out one day. I believe the specialists are getting closer – it’s just that research costs money and KD research is severely underfunded. They believe they have identified the combination of genes that make a child with KD more susceptible to the disease. And they are pretty certain that they are looking for an infectious/toxic agent that completes the perfect KD storm. I desire two things; that we can gain a greater understanding of your condition so we might have a better handle on what might be around the corner, and that the mystery of Kawasaki Disease is unravelled in our lifetime so we might gain some closure. Solving that mystery will also result in a test for the disease so that children might be diagnosed more quickly, and better treatments that further improve the possible outcomes for children with the disease.
My whole perspective on life has changed. Things I was afraid of before no longer occupy any space in my mind. I no longer sweat the small stuff. I have a lot more compassion for others – through our journey I have come into contact with so many parents who have suffered challenges with their children, KD or otherwise. Before this, I was ignorant to all that – it was happening to someone else and that didn’t matter to me. Now it does. The only fear I have now is of losing you, or losing any of the people that I love dearly. I will not allow people to hurt me anymore, because nothing can come close to the pain I have felt over the last year with you. None of that matters. Yes, everything has changed. Our lives are different than they would have been if KD hadn’t crept in. But it’s not all bad. It’s different, but not bad.
Sometimes I am scared, often I am sad. I worry a lot about the future for our little family. But above all that, you will grow up knowing that you are loved and cherished more than you could ever fathom. You are a special little girl who will achieve great things one day, and I will be there by your side with every step you take towards greatness.
I love you, Peanut.